Research on the Pathogenesis of Hemifacial Spasm through Electrophysiological Studies
Article information
Abstract
The cause of hemifacial spasm (HFS) is commonly linked to vascular compression of the facial nerve at the root exit zone. Microvascular decompression has become the most effective treatment for HFS. However, despite numerous electrophysiological studies investigating factors such as ephaptic transmission, ectopic excitation between individual nerve fibers, and hyperexcitability of the facial motor nucleus, there is still debate about the exact pathogenesis of HFS. For over 40 years, researchers have been conducting electrophysiological studies in clinical settings to better understand the pathogenesis of HFS. These studies have employed techniques including the lateral spread response, blink reflex test, facial F-waves, and transcranial electrical stimulation. Although a peripheral nerve mechanism was historically considered most likely to be responsible for this condition, recent studies are increasingly pointing to a central mechanism as the primary culprit behind HFS. This article seeks to shed light on the pathogenesis of HFS by reviewing the key findings from electrophysiological studies carried out over the years.
Introduction
Hemifacial spasm (HFS) is characterized by involuntary and irregular contractions of the facial muscles, which typically worsen over time [1]. The primary cause of HFS is believed to be vascular compression of the facial nerve at the root exit zone (REZ). Microvascular decompression (MVD) has emerged as the most effective surgical intervention for HFS [2]. Despite advancements in our understanding and treatment of HFS, there is still debate about its underlying pathogenesis, even after numerous electrophysiological studies. Two main hypotheses have been proposed to explain the mechanism of HFS: (1) the peripheral nerve mechanism, which suggests that compression of the facial nerve by a blood vessel leads to injury of the myelin sheath, promoting ectopic excitation and ephaptic transmission between nerve fibers [3-7]; and (2) the central mechanism, which posits that hyperexcitability of the facial motor nucleus (FMN), triggered by antidromically propagated discharges, induces spasms [8-11]. Researchers have investigated the pathogenesis of HFS in clinical settings using electrophysiological studies such as the lateral spread response (LSR), blink reflex test, facial F-wave, and transcranial electrical stimulation (TES). Despite four decades of research, the peripheral nerve mechanism had long been the dominant theory, but recent studies increasingly support the central mechanism as the primary driver of HFS. This article aims to consolidate and discuss the key findings from previous electrophysiological studies, providing a comprehensive overview of the progress made in understanding the pathogenesis of HFS over the last 40 years.
Electrophysiological Studies
1) Lateral spread response studies
LSR is an abnormal electromyographic finding in individuals with HFS. It is characterized by the activation of muscles innervated by branches of the facial nerve other than the one being stimulated. As such, LSR is recognized as the most distinctive electrophysiological hallmark of HFS, offering significant diagnostic value. Notably, the elimination of LSR often occurs immediately after the offending vessels are identified and adequately decompressed, especially during MVD for HFS. Consequently, LSR is used not only for diagnosis but also as a measure of MVD success. Despite numerous electrophysiological studies employing LSR to understand the pathogenesis of HFS and to ensure the effectiveness of MVD with intraoperative monitoring, there is still considerable debate about the origins of LSR within the context of HFS pathogenesis.
Several studies have been conducted on the LSR in HFS patients. Nielsen reported the presence of LSR on the symptomatic side in all 62 HFS patients he studied, particularly in the mentalis and orbicularis oculi muscles [3]. The latency of LSR was approximately 9.3 ± 0.13 ms for the orbicularis oculi and 9.0 ± 0.13 ms for the mentalis muscle. The amplitude of LSR was consistently smaller, by about 20% to 30%, than the maximal orthodromic response following facial nerve stimulation. Additionally, Nielsen and Jannetta observed changes in LSR before and after MVD surgery [5]. LSR disappeared in 23% of patients, changed from bidirectional to unidirectional in 45% within a week after MVD, and persisted in 27% of patients within 2 to 8 months post-surgery. Nielsen suggested that a peripheral mechanism, including ephaptic transmission, is the main pathogenesis for HFS, although the delayed disappearance of LSR after MVD does not rule out the hyperexcitability of the FMN as a contributing factor. To further investigate the origin of LSR, Møller and Jannetta [9] conducted analyses during MVD under anesthesia. They measured the latency of LSR from the orbicularis oculi muscle and compared it to the conduction time from the stimulation points to the facial nerve's REZ and from the REZ to the orbicularis oculi muscle. The difference in latency suggested that LSR from the orbicularis oculi muscle was not a direct result of ephaptic conduction, implicating the hyperexcitability of the FMN in the generation of LSR [6]. Studies using double stimulation and the central suppressive effect of anesthetics have also been conducted to explore the origin of LSR in HFS patients [9]. Yamashita et al. [12] used double stimulation to elicit two responses (R1 and R2) of LSR, with R1 showing consistent latency and amplitude regardless of the interstimulus intervals. Wilkinson and Kaufmann [13] investigated the effect of desflurane concentration during MVD on LSR amplitude and latency, finding a significant decrease in LSR amplitude under 1 minimum alveolar concentration desflurane with total intravenous anesthesia (TIVA). Overall, these studies aimed to understand the characteristics and origin of LSR in HFS, providing insights into the pathogenesis of this condition.
2) Blink reflex studies
The blink reflex is an electrical response associated with the clinically evoked corneal reflex. It is a true reflex, encompassing both sensory and motor components. The sensory (afferent) limb involves fibers from the supraorbital branch of the ophthalmic division of the trigeminal nerve (cranial nerve V1). The motor (efferent) limb consists of motor fibers from the facial nerve (cranial nerve VII). When the supraorbital nerve is stimulated ipsilaterally, it elicits a facial nerve response—an eye blink—on both sides. The pathway of the blink reflex includes several components within the brainstem. The afferent signal travels along the trigeminal nerve to the main sensory nucleus of cranial nerve V in the mid-pons, as well as to the nucleus of the spinal tract of cranial nerve V in the lower pons and medulla. Interneurons in the pons and lateral medulla then facilitate the nerve impulse's transmission to both the ipsilateral and contralateral facial nuclei. The efferent signal proceeds bilaterally along the facial nerve, culminating in the blink reflex. This reflex is characterized by two components: an early R1 response and a late R2 response. The R1 response occurs only on the stimulated side, while the R2 response is typically seen on both sides. The R1 response is indicative of a disynaptic reflex pathway between the main sensory nucleus of cranial nerve V in the mid-pons and the ipsilateral facial nucleus in the lower pontine tegmentum. The R2 responses are mediated by a multisynaptic pathway involving the nucleus of the spinal tract of cranial nerve V in the ipsilateral pons and medulla [14]. Considering that the blink reflex pathway encompasses the entire facial nerve, including the FMN, numerous studies have employed blink reflex testing to investigate the pathogenesis of HFS.
Nielsen [4] conducted a study on the blink reflex in 62 patients with HFS. The study found that the latency and amplitude of the R1 response on the symptomatic side were significantly higher than those on the asymptomatic side and in controls (p < 0.001). The increased latency on the symptomatic side, which was 2.1 ms longer than on the asymptomatic side, suggested focal demyelination at the site of the lesion. All patients showed a synkinetic response in the mentalis muscle on the symptomatic side, with after-activity and late-activity observed following the reflex response. These observations led to the hypothesis that ephaptic/ectopic excitation, resulting from compression and demyelination of the facial nerve, is the primary pathogenesis of HFS [4,6]. However, Esteban and Molina-Negro [10] reported different findings in their blink reflex study, which included 53 patients with HFS and compared them with healthy controls. In their study, the latency of the R1 response was similar across groups, and the latency of the R2 response was actually shorter on the symptomatic side in HFS patients, contrary to Nielsen's findings. Additionally, the duration of the R2 response was longer on the symptomatic side than on the asymptomatic side and in healthy controls. Based on these results, they proposed that the main pathogenesis of HFS was the hyperexcitability of the FMN. In a separate study by Eekhof et al. [15], blink reflex responses from the orbicularis oculi muscle showed no significant differences in latency and amplitude between HFS patients and healthy controls. However, both R1 and R2 responses from the orbicularis oris muscle were significantly more frequent and exhibited higher amplitudes on the symptomatic side in HFS patients compared to healthy controls [15]. Valls-Solé [16] investigated blink reflex responses in HFS patients using both double and single stimulation. Single stimulation revealed a larger area of R1 and R2 responses on the symptomatic side in HFS patients than on the asymptomatic side and in normal controls. With double stimulation, the inhibitory effect of conditioning stimuli on the test stimuli's R2 response, consistently seen in healthy controls, was significantly reduced at short interstimulus intervals in HFS patients. This diminished inhibitory effect suggested an increased excitability of the FMN in HFS. Møller and Jannetta [17] conducted a blink reflex study under anesthesia using inhalational anesthetics (isoflurane and nitrous oxide) during MVD. In this study, the R1 response was not evoked on the asymptomatic side under anesthesia. However, the R1 response was still observable on the symptomatic side in HFS patients under anesthesia, and this response was eliminated after MVD. These findings under anesthesia supported the conclusion that FMN hyperexcitability is the primary mechanism underlying HFS.
3) F-wave studies
F-waves represent an antidromic impulse that travels to an alpha motor neuron in the anterior horn cell of the spinal cord before returning orthodromically down the same axon. The circuitry of F-waves, which is both afferent and efferent, is exclusively motor, lacks synapses, and therefore does not constitute a true reflex. In the extremities, F-waves serve as an indicator of anterior horn cell excitability and are considered a reliable measure of lower motoneuron excitability. Facial muscles also produce measurable F-waves, which can be used to assess the excitability of the FMN. For this reason, numerous studies have employed facial F-waves to investigate the pathogenesis of HFS. Ishikawa and colleagues conducted a study with 20 patients with HFS before MVD, 10 HFS patients after MVD, and 10 healthy controls. The study aimed to explore facial F-waves obtained from the mentalis muscle by stimulating the distal mandibular branch [11]. The findings indicated that the duration of F-waves, the F/M amplitude ratio, and the frequency of F-waves on the symptomatic side of HFS patients were significantly higher compared to the asymptomatic side and healthy controls before MVD. However, there were no differences in minimum latency and chronodispersion among the groups. The study also showed that the enhancement of facial F-waves decreased concurrently with the disappearance of the LSR after MVD surgery. Another investigation by the same team compared facial F-waves from the mentalis muscle and LSR from the orbicularis oculi muscle, stimulated by the marginal mandibular branch in 10 HFS patients [18]. The study suggested that both the LSR and facial F-waves originated from the same source, as the LSR exhibited after-discharges, and the duration of these after-discharges increased on the symptomatic side. There was a linear correlation between the duration of facial F-waves and after-discharge duration, supporting the hypothesis of a common origin. Additionally, a study by Hai and Pan [19], which involved creating an HFS animal model in 10 rabbits, presented linear correlations between the amplitude ratio of LSR/M-wave and F-wave/M-wave, as well as between the duration of LSR and F-waves. The researchers concluded that the increase in facial F-wave duration in HFS could not be solely attributed to peripheral mechanisms, including ephaptic transmission [20]. Ishikawa et al. [21] further conducted a study involving facial F-waves, blink reflexes, and LSR before and after MVD in 20 HFS patients. The findings showed increased values of facial F-waves and blink reflex on the symptomatic side before MVD. Additionally, facial F-waves and LSR were still recorded in some patients within one month after the complete disappearance of HFS symptoms, suggesting that hyperexcitability of the FMN could be the primary cause of HFS.
4) Transcranial facial motor evoked potential studies
Transcranial motor evoked potentials (TcMEPs) represent a highly effective method for intraoperative monitoring, particularly during spine surgery, to assess motor function. These potentials are obtained by stimulating motor pathways situated above the surgical site. The activation of these pathways is measured by recording waveforms as the impulse travels down the corticobulbar and corticospinal tracts. Similar to the blink reflex, a TcMEP study can be a valuable tool for examining the entire efferent pathway of the facial nerve. Although not commonly performed, some researchers have suggested using myogenic facial motor evoked potentials (FMEPs) elicited through TES to monitor the functional integrity of the corticobulbar tract, FMN, and facial nerve during MVD surgery. Wilkinson and Kaufmann [22] conducted a study that measured FMEPs with the LSR during MVD in 10 patients with HFS and performed FMEP studies during MVD for 17 patients with trigeminal neuralgia (TN). The analysis included parameters such as latency, amplitude, and duration of FMEP before and after MVD. The results indicated a significant decrease in the amplitude and duration of FMEPs on the symptomatic side of HFS patients after MVD, with no such changes observed on the asymptomatic side of HFS patients or in TN patients. They also noted a marked reduction in FMEP amplitude and duration coinciding with the disappearance of LSR during decompression of the offending vessel. However, there was no significant change in the latency of FMEPs before and after MVD. Another retrospective analysis compared the FMEP threshold and the incidence of FMEPs to single-pulse TcMEPs during surgery in 65 HFS patients and 29 patients with skull base tumors [13]. The study found significantly lower FMEP thresholds in HFS patients than in those with skull base tumors, and FMEP responses to single-pulse stimulation were observed in 87% of HFS patients, while only 10% of skull base tumor patients exhibited FMEP responses. In a more recent prospective study, Wilkinson et al. [23] compared FMEPs under TIVA with or without desflurane during MVD for HFS patients to understand the hyperexcitability of the FMN in HFS. They hypothesized that there would be differences in the effect of desflurane on FMEPs between the symptomatic and asymptomatic sides, given the suppressive effects of inhalational anesthetics on alpha motor neurons. The study suggested that the suppressive effects of desflurane were less pronounced on the symptomatic side than on the asymptomatic side, indicating that hyperexcitability of the FMN is a key factor in the pathogenesis of HFS.
Conclusion
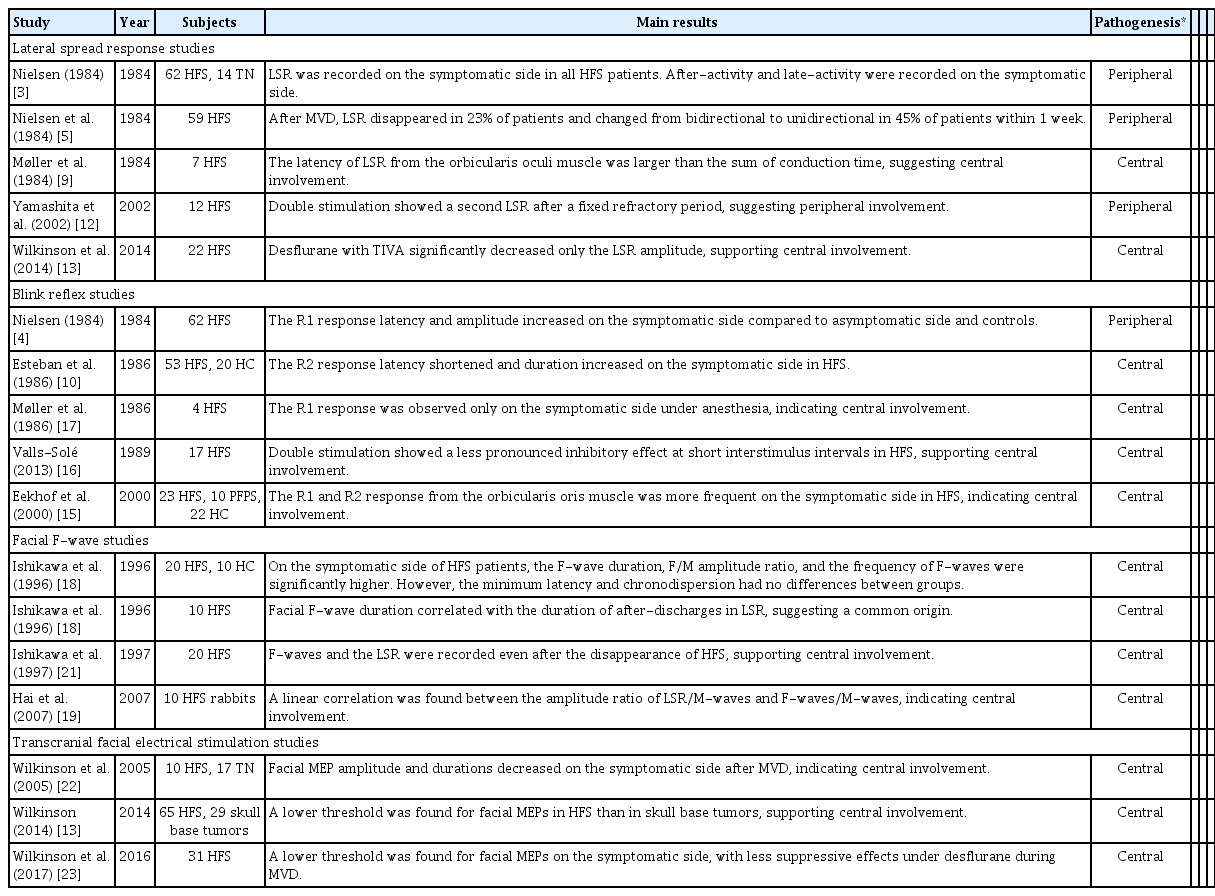
The pathogenesis of HFS has long been debated, with discussions centering on whether it originates from ephaptic transmission/ectopic excitation among individual nerve fibers or from the hyperexcitability of the FMN. A variety of electrophysiological techniques, including the LSR, blink reflex tests, facial F-waves, and TcMEPs, have been employed in numerous studies to investigate the pathogenesis of HFS (Table 1). The accumulation of findings and the evolution of research methods have substantially improved our understanding of HFS pathogenesis. Based on the collective evidence from previous studies, hyperexcitability of the FMN is considered to be the main mechanism involved in the pathogenesis of HFS.
Notes
Conflict of Interest
No potential conflict of interest relevant to this article was reported.